 
When the design is to deliver increased pressures, inflations, or “breaths” superimposed on the continuous positive pressure, this is termed NIPPV or NIMV (nasal intermittent mandatory ventilation). 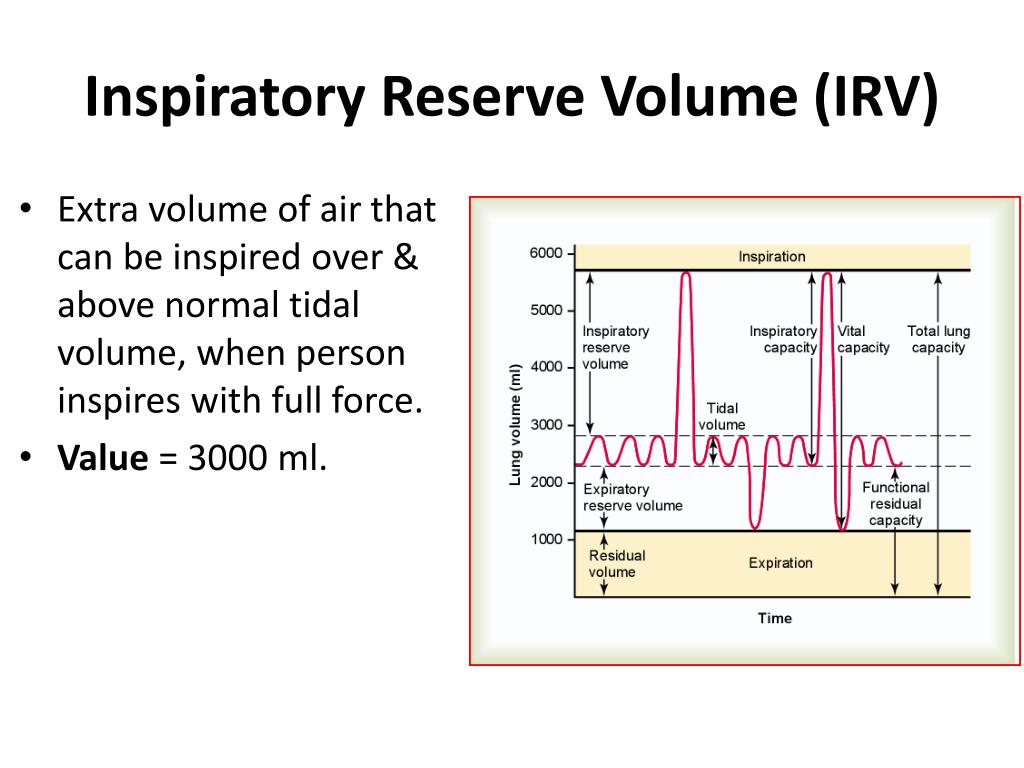
When the strategy involves a device delivering a constant distending pressure to the airways via a nasal interface, this is termed NCPAP. These non-invasive forms of respiratory support include nasal continuous positive airway pressure (NCPAP) and nasal intermittent positive pressure ventilation (NIPPV).īoth NCPAP and NIPPV have been broadly defined and actually describe a range of devices and interfaces that can be grouped according to two different strategies. To avoid these complications of mechanical ventilation, methods to support infants without endotracheal tubes have been developed. While potentially life-saving, prolonged invasive mechanical ventilation is associated with substantial healthcare cost and a variety of pulmonary and extra-pulmonary complications including air leak syndromes, traumatic injury to the large airways, retinopathy of prematurity, and bronchopulmonary dysplasia. Delivoria-Papadopoulos and Swyer described the use of endotracheal tubes to provide positive pressure ventilation to neonates in 1963. Mechanical ventilation of the preterm newborn with respiratory insufficiency or respiratory failure has become one of the mainstays of neonatal care since Drs. NIPPV via RAM cannula produces minimal, clinically insignificant tidal volumes during non-spontaneous inflations. both ventilator-assisted and unassisted efforts). Tidal volumes during ventilator-only inflations were 0.06 ± 0.04 ( p < 0.005 vs. Mean tidal volumes in arbitrary units were 0.30 ± 0.22 in NIPPV inflations associated with patient effort and 0.27 ± 0.15 in spontaneous breaths without ventilator assistance ( p = 0.82). We compared tidal volumes during ventilator-supported breaths, unsupported breaths, and ventilator inflations not accompanied by patient effort (defined using electrical activity of the diaphragm). Design/Methodsįourteen subjects were monitored while receiving NIPPV. 
We tested the hypothesis that inflations delivered with NIPPV via RAM ® cannula and not accompanied by patient effort produce minimal tidal volume as measured by respiratory inductance plethysmography. It is about 6000 ml.Nasal intermittent positive pressure ventilation (NIPPV) is a widely used mode of support in neonates, during which ventilator inflations may or may not coincide with spontaneous breathing. Total lung capacity- Maximum amount of air that can be held at any time in the two lungs, called total lung capacity. The average Residual Volume (RV) in healthy males is about 1200 ml. Residual volume- The volume of air that remains in the lungs even after maximum or forceful expiration. Vital capacity- The maximum amount of air a person can expel from the lungs after a maximum inhalation. Expiratory reserve volume- The expiratory reserve volume (ERV)is the additional air that can be forcibly exhaled after the expiration of a normal tidal volume. It is the additional air that can be forcibly inhaled after the inspiration of a normal tidal volume.ĥ. Inspiratory reserve volume- The inspiratory reserve volume (IRV), about 3,000 mL. Alveolar air- The tidal volume contained in alveoli. Dead air space- Some of the air in the trachea and bronchi do not take part in breathing, called dead air space. Tidal volume- The amount of air breathed in and out in normal quiet breathing. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
